
Introduction
Administrative inefficiencies drain an estimated $351 billion annually from the U.S. healthcare system, with physicians spending nearly half their clinic day on EHR documentation and desk work rather than patient care. Manual processes—from patient intake and insurance verification to claims routing and follow-up calls—create costly bottlenecks that contribute to staff burnout and revenue leakage.
No-code and open-source automation platforms directly address that revenue and productivity gap. Non-technical staff can build compliant, automated workflows without waiting months for IT or expensive custom development. Clinics, hospitals, and healthtech teams deploy solutions in weeks rather than quarters—targeting high-friction workflows while maintaining HIPAA compliance.
This guide covers which workflows to automate first, how no-code and open-source platforms differ, and what HIPAA compliance actually requires from these tools.
TL;DR
- Healthcare automation eliminates repetitive tasks, cutting costs and reducing staff burnout
- No-code platforms offer visual drag-and-drop building; open-source platforms give regulated environments full data sovereignty
- Automate patient intake, scheduling, insurance verification, EHR updates, and follow-ups first
- HIPAA compliance requires BAAs, encryption, audit trails, and role-based access controls
- Choose your platform based on who controls your data — not just who offers the most features
What Is Healthcare Automation?
Healthcare automation uses digital tools and software logic to handle repetitive, rule-based tasks across clinical and administrative workflows without manual intervention for each step. This encompasses everything from routing lab results to triggering billing notifications to sending appointment reminders.
Three tiers of automation tools exist:
- No-code platforms — Drag-and-drop visual interfaces requiring zero coding, built for non-technical staff (for example, Kissflow, Microsoft Power Automate, Quickbase)
- Low-code platforms — Some configuration or scripting required, faster than full development but needs technical oversight
- Open-source/self-hosted platforms — Full control over data and infrastructure, customizable, suitable for regulated environments (for example, n8n, ActivePieces)

Adoption is accelerating across industries. Gartner forecasted that 70% of new enterprise applications would use low-code or no-code technologies by 2025, up from less than 25% in 2020. For healthcare specifically, these platforms address a concrete pressure point: administrative tasks now consume nearly half of a physician's working day, leaving less time for direct patient care.
Healthcare Workflows That Benefit Most from Automation
Focus on high-friction, high-volume workflows where automation delivers fast, measurable ROI. These areas consume the most staff time and create the greatest operational bottlenecks.
Patient Intake and Appointment Scheduling
Manual intake—paper forms re-entered into EHR systems—and phone-based scheduling waste significant staff time. In 2024, physicians reported working 57.8 hours per week, with 7.3 hours dedicated specifically to administrative tasks like prior authorization and insurance forms.
What automated intake delivers:
- Secure digital forms that feed directly into EHR systems
- Tokenized links for mobile-friendly access
- Rules-based booking systems syncing with existing calendars
- Prevention of double bookings through real-time availability checks
Automated reminders (SMS and telephone) increase outpatient attendance by 11% compared to usual care, reducing no-show rates and maximizing provider capacity.
Insurance Verification, Billing, and Revenue Cycle
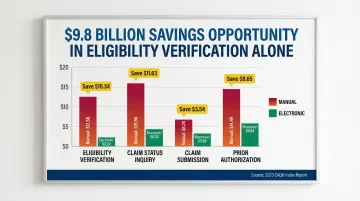
Staff manually logging into multiple payer portals, chasing denials, and routing claims create billing backlogs and revenue leakage. Cost comparison of manual vs. electronic transactions (medical providers):
| Transaction Type | Manual Cost | Electronic Cost | Industry Savings Opportunity |
|---|---|---|---|
| Eligibility Verification | $12.56 | $2.22 | $9.8 billion |
| Claim Status Inquiry | $15.96 | $4.33 | $3.22 billion |
| Claim Submission | $6.74 | $3.20 | $2.07 billion |
| Prior Authorization | $14.49 | $5.84 | $494 million |
Source: 2023 CAQH Index Report
Eligibility verification represents the largest single savings opportunity at $9.8 billion annually if fully automated. No-code automation can connect to clearinghouse APIs (Availity, Change Healthcare) to verify eligibility in real time, auto-route denied claims, and trigger billing team notifications—all without manual portal logins.
EHR Updates, Lab Results, and Clinical Workflows
Automating clinical workflows removes staff from the middle of routine data handoffs. Key capabilities include:
- Generating lab orders directly from EHR diagnosis codes
- Delivering results to patients via secure portals automatically
- Flagging critical values to care teams without manual review
- Syncing data bidirectionally between clinical tools (Epic, Cerner, Oracle Health) and workflow apps
A 2025 JAMIA Open study found that FHIR-based EHR-to-EDC integration increased data entry speed by 58% and reduced transcription errors by 99% compared to manual entry. Low-code/no-code platforms with FHIR/HL7 integration make this level of automation achievable without custom code.
According to a 2025 ONC data brief, 70% of non-federal acute care hospitals now enable patient access using apps configured to meet HL7 FHIR specifications, making API-based automation viable across most health systems today.
Post-Visit Follow-Ups and Patient Communication
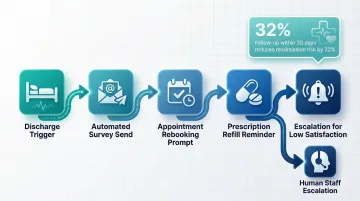
Outpatient follow-up within 30 days of discharge reduces readmission risk by 32%—yet a 2025 Medicare analysis found that 42.5% of patients discharged directly home lacked timely follow-up. That gap is largely a staffing and capacity problem automation can solve.
Automated follow-up workflows include:
- Trigger-based survey sends after visits
- Appointment rebooking prompts
- Prescription refill reminders
- Escalation logic for low patient satisfaction scores
Automated outreach does have limits in complex care scenarios. A 2023 randomized trial (MESSAGE-HF) found that automated SMS messaging improved heart failure self-care scores but failed to reduce 180-day readmissions or mortality.
The takeaway: automation handles routine communications well. Complex clinical interventions still require human judgment.
No-Code vs. Open-Source Platforms: Which Fits Healthcare Best?
The right platform depends on team size, technical capability, compliance needs, and whether your organization must keep PHI on-premise.
No-Code Commercial Platforms
Strengths:
- Fast setup with pre-built healthcare templates
- FHIR connectors for EHR integration
- Drag-and-drop interfaces empowering non-technical staff
- Managed infrastructure with vendor support
Limitations:
- Vendor lock-in
- Recurring platform fees (often per-user or per-transaction)
- Data stored on third-party cloud infrastructure
- Limited customization beyond template features
Key selection criteria for healthcare use:
- Vendor signs Business Associate Agreement (BAA)
- Supports role-based access controls
- Documented HIPAA-compliant configurations
- Encryption at rest and in transit
BAA availability varies significantly:
| Platform | BAA Status | Requirements |
|---|---|---|
| Zapier | Not eligible | No HIPAA compliance on any plan |
| Airtable | Eligible | Enterprise Scale Plan only |
| Slack | Eligible | Enterprise Grid plan only |
Open-Source and Self-Hosted Platforms
Open-source tools (n8n, ActivePieces) offer full visibility into the codebase, no platform fees, and the ability to self-host on your own infrastructure, giving healthcare organizations complete data sovereignty over PHI.
Core advantages:
- Full source code access for security audits
- No recurring platform fees beyond infrastructure costs
- Self-hosting on private cloud or on-premise servers
- Complete control over data residency and processing
- Customizable to specific compliance requirements
That same data sovereignty extends to patient-facing phone communication — appointment reminders, call answering, and intake — where PHI exposure risk is high. Platforms like Dograh AI apply this self-hosted, open-source model directly to voice: HIPAA-compliant, 24/7 automated call handling with no-code agent deployment and a full audit trail, all running on infrastructure you control.
One tradeoff to plan for: open-source and self-hosted tools require more initial setup and DevOps support than managed no-code SaaS. That makes them best suited for organizations with internal technical capacity or a relationship with a compliant hosting partner.
Side-by-Side Comparison
| Feature | No-Code Commercial | Open-Source/Self-Hosted |
|---|---|---|
| Deployment | Cloud (vendor-managed) | Self-hosted or cloud |
| HIPAA BAA | Varies by vendor/plan | Self-hosting eliminates BAA dependency |
| Coding Required | None | Low to moderate (initial setup) |
| Cost Model | Subscription/per-user | Open-source (infrastructure only) |
| Data Control | Third-party managed | Full organizational control |
| Best For | SMB, rapid deployment | Enterprise, regulated environments, data sovereignty |

HIPAA Compliance: What No-Code and Open-Source Platforms Must Deliver
HIPAA compliance in automation is not automatic. Any workflow touching Protected Health Information (PHI) must meet specific technical and administrative safeguards, regardless of whether the platform is no-code or open-source.
Essential Technical Requirements
Under 45 CFR 164.312 Technical Safeguards, automation platforms handling ePHI must implement:
- End-to-end encryption covering data at rest and in transit
- Role-based access controls with unique user identification and automatic logoff
- Multi-factor authentication to verify user identity before access
- Audit logging that records and examines all activity across information systems
Low-code/no-code platforms meeting these standards can actually exceed traditional development in consistency of enforcement, as controls are built into the platform rather than implemented per-project.
Business Associate Agreement (BAA) Requirement
Failure to execute a BAA carries severe penalties. In 2016, North Memorial Health Care paid $1.55 million to OCR for failing to implement a BAA with a major contractor and failing to institute an organization-wide risk analysis.
Consumer-grade versions of popular tools are typically not BAA-eligible: Standard Zapier, Airtable free tier, and Slack all require enterprise plans or explicitly do not support HIPAA compliance. For organizations that cannot navigate those enterprise requirements, self-hosting is a direct alternative.
Self-Hosted Deployment Eliminates Third-Party BAA Dependency
Self-hosted, open-source deployment eliminates third-party BAA dependency entirely, since PHI never leaves the organization's own infrastructure. This is the preferred approach for government health systems and large hospital networks that cannot risk third-party data exposure.
Operational Compliance Best Practices
Compliance is also operational, not just technical:
- Shadow testing before production deployment
- Human-in-the-loop checkpoints for high-risk workflows
- Phased rollouts starting with low-risk processes
- Continuous monitoring and audit review
- Regular access control reviews
- Incident response procedures

How to Implement Healthcare Automation Without Disrupting Operations
Practical Starting Framework
1. Audit high-friction workflows Identify manual tasks consuming the most staff time. Survey frontline staff (nurses, care coordinators, billing teams) to understand real friction points.
2. Prioritize one measurable pilot Start with a single workflow like automating patient intake forms or eligibility verification. Choose something with clear success metrics (time saved, error reduction, cost per transaction).
3. Establish governance Define data loss prevention policies, access controls, and a center of excellence or internal owner before scaling. Assign accountability for monitoring, updating, and optimizing workflows.
Speed Advantage: LCNC vs. Custom Development
According to Health Tech Magazine, traditional EHR custom workflows take 6-12 months to deliver, while LCNC development compresses this to 4-8 weeks. Texas Children's Hospital used Microsoft Power Apps to move from idea to pilot in that same window, deploying supply chain bots and nursing leadership assessment tools while maintaining IT governance and HIPAA compliance.
Stakeholder Alignment
Involve frontline staff in workflow design. They understand the real friction points and will be the primary users. Prioritize adoption through training and support resources, not just technical deployment.
Turning that intent into adoption means building the right support infrastructure:
- Provide clear documentation and role-specific reference guides
- Run hands-on training sessions before and after go-live
- Create a structured feedback loop so staff can flag friction early
Frequently Asked Questions
What is no-code healthcare workflow automation?
No-code healthcare workflow automation uses visual, drag-and-drop platforms to automate clinical and administrative processes—like intake, scheduling, and billing—without requiring programming skills, making it accessible to non-technical healthcare staff.
How is RPA used in healthcare workflow automation?
Robotic Process Automation (RPA) automates repetitive, rules-based tasks by mimicking user interactions with existing software—entering data into payer portals, extracting lab results, or processing claims. It's commonly paired with no-code platforms to extend automation to legacy systems that lack APIs.
What are the main HIPAA compliance requirements for healthcare automation platforms?
Core requirements include end-to-end encryption (at rest and in transit), role-based access controls, audit logging, multi-factor authentication, and a signed Business Associate Agreement (BAA) with any vendor handling PHI.
What is the difference between no-code and open-source healthcare automation platforms?
No-code platforms offer managed, cloud-based tools with visual builders requiring zero coding. Open-source platforms provide full source code access and self-hosting options, giving organizations complete data control—particularly valuable in HIPAA-regulated environments.
Can voice AI be HIPAA-compliant for patient communication?
Yes, provided the platform supports self-hosting or offers a signed BAA, encrypts call data, and maintains full audit trails. Self-hosted voice AI solutions avoid third-party data exposure, making them well-suited for healthcare communication automation.
Which healthcare workflows deliver the fastest ROI from automation?
Patient intake, appointment scheduling, and insurance eligibility verification typically deliver the fastest returns. Eligibility verification alone represents a $9.8 billion annual savings opportunity across medical and dental industries. Medical providers save an average of 16 minutes and $10.34 per transaction when the process is automated.


