
Introduction
Healthcare scheduling isn't retail booking or restaurant reservations—it's a clinical, financial, and emotional coordination challenge where a single missed call can delay treatment, not just disappoint a customer. Medical practices miss an average of 42% of incoming calls during business hours, and each missed appointment costs approximately $200, contributing to a staggering $150 billion annual loss for the U.S. healthcare system.
The core tension healthcare providers face today is clear: traditional phone-based and manual scheduling systems are cracking under relentless patient demand, widespread staff shortages, and growing after-hours volume. Front-desk staff turnover reached 40% in 2022, leaving remaining teams stretched thin between check-ins, clinical messaging, and ringing phones.
This article explains how conversational AI is the operational answer to that pressure. You'll learn what it actually is, how it works from first contact through confirmation, the measurable benefits for providers and patients, what HIPAA compliance truly requires, and how to choose a platform built for healthcare's unique demands.
TLDR:
- Healthcare practices miss 42% of calls, costing $200 per unfilled appointment and $150 billion annually nationwide
- Conversational AI uses Natural Language Processing to handle scheduling 24/7 via phone or text, capturing after-hours demand
- AI systems integrate with EHR calendars in real-time, book appointments directly, and cut no-shows by 11% through automated reminders
- HIPAA compliance requires Business Associate Agreements and secure data handling—self-hosting options give maximum control over patient data
- The right platform handles medical terminology, responds in under 500ms, and escalates to human staff when needed
Why Traditional Healthcare Appointment Scheduling Falls Short
Traditional phone-based scheduling creates specific, measurable failure modes that ripple across an entire practice.
Each failure mode is measurable — and costly:
- Call abandonment: At least 60% of patients abandon calls after one minute on hold, and 85% won't call back after an unanswered first attempt. For a call center handling 2,000 daily calls, revenue losses can reach $45,000 per day.
- Staff bottlenecks: Front-office staff spend 31% of their phone time on scheduling alone — second only to eligibility and prior authorization work. When a patient at the desk and a caller on hold compete for attention, the caller loses.
- No after-hours access: Traditional systems operate during business hours only. Between 34–51% of appointments could be scheduled outside standard hours if self-service tools were available. Without that access, those slots go unfilled.
- Rigid IVR systems: Basic phone trees rely on static decision logic that can't adapt to real-time availability changes, insurance status, or provider-specific rules — and can't understand natural language, forcing patients through frustrating menu mazes.

These failures don't stay isolated. Patients who can't get through delay or abandon care entirely. Front-desk staff burn out handling repetitive calls instead of higher-value clinical work. No-show rates climb when confirmations and reminders stay manual. The average no-show rate across medical specialties sits at approximately 23%, with primary care averaging 19%.
What Is Conversational AI for Healthcare Appointment Scheduling?
Conversational AI for healthcare scheduling refers to AI systems that use Natural Language Processing (NLP) and voice or text interfaces to simulate human-quality dialogue, allowing patients to book, reschedule, and cancel appointments through natural conversation rather than menus or forms.
How It Differs from Basic Automation
Unlike basic chatbots or IVR systems that follow fixed scripts, conversational AI platforms understand intent, handle ambiguity in natural speech, retain context across multi-turn conversations, and respond dynamically. Rules-based systems use "if-then" decision trees; NLP-powered systems interpret meaning.
When a patient says "I need to see Dr. Martinez sometime next week, preferably in the afternoon," a traditional IVR fails entirely. Conversational AI extracts the provider name, timeframe, and preference automatically — no menu navigation required.
Primary Delivery Modes in Healthcare
- Voice AI handles inbound calls in real-time spoken conversation — especially relevant because most patients still call to schedule, including older populations and those with urgent needs.
- Text/Chat AI operates through web chat widgets, SMS, or messaging apps like WhatsApp, serving patients who prefer asynchronous communication.
The scale of adoption reflects genuine demand. Gartner defines conversational AI platforms as products that leverage composite AI, including generative AI and natural language technologies, to simulate human conversation. The global conversational AI in healthcare market was valued at $13.68 billion in 2024 and is projected to reach $106.67 billion by 2033.
What Conversational AI Is Not
It is not ambient clinical documentation AI, not predictive analytics for patient risk, and not a full replacement for clinical staff. Its role is to automate the administrative layer of patient access so human staff can focus on complex or sensitive interactions that require empathy, clinical judgment, or exception handling.
How Conversational AI Handles the Full Scheduling Lifecycle
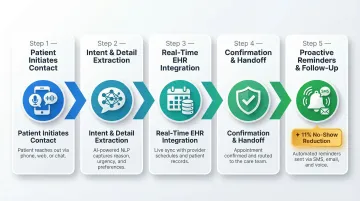
Step 1 — Patient Initiates Contact
A patient calls the practice at 9 p.m., well after business hours. The AI agent answers instantly with a natural greeting: "Hello, you've reached Dr. Chen's office. How can I help you today?"
The AI identifies the reason for contact—new appointment, reschedule, cancellation, or general inquiry—through open-ended conversational dialogue, not a menu. The patient says, "I need to reschedule my Thursday appointment," and the AI understands immediately.
Step 2 — Intent and Detail Extraction
The AI extracts key scheduling variables through natural back-and-forth conversation:
- Preferred provider and specialty
- Desired date and time window
- Urgency level
- Insurance information
NLP handles dialect variation, incomplete sentences, and implied intent. When a patient says "sometime this week if possible," the system interprets urgency and flexibility — no rigid form-filling or exact phrasing required.
Step 3 — Real-Time EHR and Calendar Integration
With intent captured, the AI queries the practice's scheduling system or EHR in real-time to check provider availability, apply specialty- or location-specific booking rules, and surface valid appointment slots.
Modern platforms integrate using HL7 FHIR standards — specifically the Appointment, Schedule, and Slot resources — ensuring compatibility with major EHR systems. Double-bookings and incorrect slot assignments are eliminated at the source.
Step 4 — Confirmation and Handoff
Once the slot is confirmed, the AI books it directly into the calendar, sends confirmation via SMS or voice, and logs the full interaction for staff review.
For complex clinical needs—such as a patient mentioning chest pain or asking detailed medication questions—the AI escalates intelligently to a human staff member, passing a complete context summary so the patient doesn't repeat themselves.
Step 5 — Proactive Reminders and Follow-Up
Booking confirmation isn't the end of the workflow. The AI handles outbound follow-through as well:
- Automated appointment reminders via SMS or voice call
- No-show follow-up calls
- Rescheduling prompts to fill cancelled slots
Research shows that SMS and telephone reminders significantly improve outpatient appointment attendance rates by 11% compared to no reminders. For a busy practice, that 11% attendance lift translates directly to fewer revenue gaps and more consistent patient care.
Key Benefits for Providers and Patients
Operational Benefits for Healthcare Providers
24/7 Availability Without Staffing Costs
The AI handles inbound scheduling around the clock, capturing after-hours and weekend calls that previously went to voicemail. Studies show 34-51% of appointments can be scheduled outside standard office hours when patients have self-service access — meaning more booked appointments and fewer missed calls.
Staff Reallocation and Reduced Burnout
Front-desk staff are freed from repetitive call handling to focus on check-in, clinical support, and tasks requiring human judgment. Scheduling consumes 31% of staff phone time, so that's a meaningful productivity return. Replacing a frontline staff member costs $25,000-$30,000 — reducing that administrative burden directly lowers the burnout-driven turnover that makes retention so costly.
Faster Scheduling Cycles and Higher Calendar Utilization
AI systems fill open slots and canceled appointments faster by simultaneously managing inbound requests and proactive outreach. This reduces idle capacity — particularly in specialty care where equipment and staffing costs make unused time expensive.
Patient Experience Benefits
Frictionless Access to Care
Patients book when it's convenient — late evening, early morning, or between meetings — without hold music or callback queues. Longer telephone wait times decrease patients' perceived ability to access urgent care appointments in a timely manner, which hits satisfaction scores directly. That connection matters: 80% of healthcare consumers say online scheduling influences their choice of provider.
Reduced Barriers for Diverse Patient Populations
Multilingual NLP capabilities let conversational AI serve patients in their preferred language — a meaningful access issue. Approximately 25.7 million people in the U.S. have Limited English Proficiency (LEP), and 25% of adults with LEP report that language barriers made it difficult to schedule a medical appointment.
HIPAA Compliance, Data Security, and Self-Hosting
Healthcare scheduling AI carries specific compliance obligations because every patient interaction—name, condition, insurance, appointment type—is Protected Health Information (PHI) under HIPAA.
What Qualifies as PHI
Under the HIPAA Privacy Rule, PHI covers all "individually identifiable health information" held or transmitted by a covered entity or business associate. This includes demographic data tied to a patient's past, present, or future physical or mental health.
Scheduling data falls squarely within this definition. Appointment types, provider names, and insurance details linked to a patient's name or IP address all constitute PHI.
Business Associate Agreements
Any AI system handling PHI requires a signed Business Associate Agreement (BAA) before deployment. Under 45 CFR 164.504(e), a compliant BAA must:
- Define permitted uses of PHI by the vendor
- Require appropriate safeguards (encryption in transit and at rest, access controls, audit logging)
- Mandate breach reporting for any unauthorized use or disclosure
Self-Hosting as a Compliance Differentiator
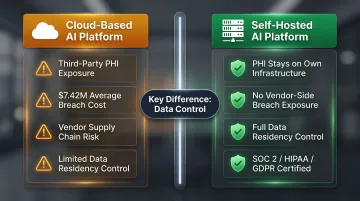
Cloud-based AI platforms require trusting a third-party vendor with PHI — and that trust carries real financial risk. The average healthcare data breach costs $7.42 million, well above the $4.44 million global average, and 15% of initial attack vectors involve supply chain or vendor breaches.
Self-hostable platforms like Dograh AI let health systems deploy voice AI on their own infrastructure — giving complete control over where patient data resides and removing vendor-side breach exposure entirely. Dograh AI carries SOC 2, HIPAA, GDPR, and PCI DSS certifications, with both cloud and on-premise deployment options available.
When evaluating AI scheduling platforms, verify:
- HIPAA compliance with an available, signed BAA
- Whether your data trains external models or is shared with third parties
- Data residency — where exactly PHI is stored and processed
- Audit logging capabilities for compliance reporting and breach investigation
Choosing the Right Conversational AI Scheduling Platform
Core Technical Requirements
Any platform worth evaluating must check these boxes before you go further:
- Genuine NLP — not scripted menus — to understand natural patient language and intent, including variations in how patients describe symptoms or specialties
- Real-time EHR and calendar integration that queries live availability and books directly, without manual re-entry between systems
- Sub-500ms total voice latency (STT + LLM + TTS combined); delays beyond 200-300ms become noticeable and erode the experience fast
- Practice-specific scheduling logic covering provider booking windows, specialty routing, location-based availability, and insurance type filters

Deployment and Total Cost Considerations
Watch for platforms that layer per-call or per-minute fees on top of LLM, STT, and TTS costs — that combination makes expenses unpredictable at scale. Some proprietary platforms charge $0.05/minute in platform fees alone, with separate STT, LLM, and TTS charges stacked on top, pushing total costs to $0.23–$0.33/minute.
Transparent pricing without double billing is the alternative. Dograh AI's open-source model lets organizations use their own API keys with no platform markup, so the cost structure stays visible from day one.
Beyond cost, deployment speed matters more than most buyers anticipate. Two areas to evaluate:
- Time-to-production — platforms that launch in days rather than months cut implementation risk significantly. Dograh AI's framework can deploy a base voice agent in 2 minutes, though full healthcare rollout timelines vary with EHR integration complexity and compliance validation.
- Ongoing configurability — can staff update scheduling rules, provider availability, or escalation logic without filing a support ticket?
Evaluation Criteria Specific to Healthcare
Medical terminology and pronunciation:
Confirm the vendor understands medical terminology and provider name pronunciation. Misunderstood specialty names or mispronounced provider names damage patient trust immediately.
Full conversation audit logs:
HIPAA compliance reporting requires detailed audit trails showing who accessed what patient data and when. Verify the platform provides complete conversation transcripts, audit logs for workflow edits, and role-based access control (RBAC) for sensitive data.
Graceful escalation to human staff:
The platform must support intelligent escalation logic: when a patient asks a clinical question, expresses urgency, or the AI cannot resolve the request, it should transfer to a human staff member with a full context summary so the patient doesn't repeat themselves.
Frequently Asked Questions
How can AI help with appointment scheduling?
AI scheduling systems use Natural Language Processing to handle patient calls and messages 24/7, book appointments directly into the EHR, and send confirmations and reminders automatically. This reduces missed appointments, improves patient access, and frees front-desk staff from repetitive call-handling tasks.
Which AI tool can automate scheduling meetings in healthcare?
Voice AI platforms designed for healthcare—such as Dograh AI—can fully automate inbound appointment calls, reschedule and cancellation requests, and outbound reminders while remaining HIPAA-compliant and integrating with existing EHR systems through HL7 FHIR standards.
Is conversational AI for healthcare appointment scheduling HIPAA-compliant?
Compliance depends on the platform. Look for vendors offering a Business Associate Agreement (BAA), encrypted data handling in transit and at rest, and self-hosting options that keep PHI on the organization's own infrastructure rather than third-party cloud servers.
Can conversational AI integrate with existing EHR systems?
Yes. Leading conversational AI scheduling platforms integrate with major EHR systems using HL7 FHIR standards to check real-time provider availability, apply specialty-specific scheduling rules, and book appointments directly into the calendar without manual data re-entry or double-booking risks.
What happens when a patient's request needs a human staff member?
Well-designed conversational AI systems include intelligent escalation logic. When a patient asks a clinical question, expresses urgency or distress, or the AI cannot resolve the request, it transfers to a human staff member with a full context summary covering patient details, conversation history, and the specific issue — so the patient never has to repeat themselves.


