](https://file-host.link/website/dograh-ypucar/assets/blog-images/eb895f01-e0b8-4af8-a641-dadf85b112ad/1776198164376524_0d3dec270bd94433b9d65f2f49fc3ed7/360.webp)
Introduction
Missed appointments drain $150 billion from U.S. healthcare annually, with each vacant 60-minute slot costing physicians roughly $200. Traditional reminder calls by staff are expensive—medical secretaries average $21.91 per hour nationally—slow, inconsistent, and create compliance risk when patient data passes through multiple hands or systems.
HIPAA-compliant conversational AI automates outreach across voice, SMS, and chat while keeping Protected Health Information (PHI) secure. Unlike rigid Interactive Voice Response (IVR) menus that suffer 35-45% abandonment rates, modern conversational AI understands natural language ("I need to reschedule") and reduces no-shows by 30% or more.
This guide covers what you need to deploy appointment reminders that protect patients and your practice:
- HIPAA compliance requirements and technical safeguards
- How conversational AI reduces no-show rates
- EHR integration approaches
- Vendor selection criteria
TLDR
- Appointment reminders contain PHI (patient name, date, provider), triggering HIPAA's administrative, physical, and technical safeguard requirements
- A signed BAA with your AI vendor is legally required; OCR fined Pagosa Springs Medical Center $111,400 for skipping this step
- Conversational AI automates confirmations, rescheduling, and follow-ups across the full appointment lifecycle
- Data must be encrypted in transit (TLS 1.3, SRTP) and at rest (AES-256) to meet HIPAA technical safeguards
- EHR integration with write-back capability prevents double-booking and eliminates manual status updates
- Self-hosting options give organizations complete data sovereignty and compliance control
Why Appointment Reminders Are a HIPAA Compliance Risk
What Qualifies as PHI in Reminders
Even a simple reminder containing a patient name, appointment date, provider name, or appointment type qualifies as PHI under 45 CFR 160.103. Each of these individually identifiable elements relates to healthcare provision — bringing every automated reminder under HIPAA's Security and Privacy Rules.
The Financial Stakes Are Enormous
Healthcare data breaches remain the costliest across all industries. The 2025 IBM Cost of a Data Breach Report shows healthcare breaches average $7.42 million per incident, while U.S. breaches of any kind average $10.22 million — the highest globally.
OCR enforces a tiered penalty structure for HIPAA violations. Adjusted for inflation in 2024, maximum penalties for uncorrected willful neglect reach $73,011 per violation, with annual caps of $2,190,294 per violation category. OCR has already levied significant fines for exactly this type of failure:
| Organization | Penalty | Core Failure |
|---|---|---|
| Pagosa Springs Medical Center | $111,400 | Disclosed ePHI of 557 patients to a web-based scheduling vendor without a BAA |
| Center for Children's Digestive Health | $31,000 | Stored PHI with a vendor without a signed BAA |
| University of Rochester Medical Center | $3,000,000 | Failed to encrypt ePHI, leading to loss of unencrypted devices |

Compliance Covers the Entire Communication Path
Those penalties make one thing clear: the risk isn't limited to data storage. HIPAA governs how PHI moves in real time across every channel, including voice calls and SMS.
Each component of an AI platform's communication infrastructure is a potential exposure point:
- Encryption protocols governing data in transit between systems
- Carrier connectivity handling the call path from origination to termination
- Audio streaming between the telephony layer and AI inference
If any segment of that path — from carrier edge to AI inference layer — runs unencrypted, PHI is exposed during transmission. Selecting a platform that secures the full call path, not just the database, is non-negotiable.
What HIPAA-Compliant Conversational AI for Appointment Reminders Actually Does
Core Definition
HIPAA-compliant conversational AI for appointment reminders is an automated system—voice agent or chatbot—that communicates with patients in natural language about their appointments (confirming, rescheduling, following up) while enforcing all required PHI protections throughout the process.
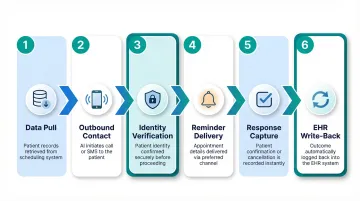
The Standard Reminder Workflow
- Data pull: AI retrieves appointment data from the scheduling system or EHR
- Outbound contact: System initiates contact at a configured time before the visit (e.g., 72 hours prior)
- Identity verification: AI verifies patient identity before disclosing any PHI
- Reminder delivery: System delivers appointment details in natural language
- Response capture: AI captures patient response—confirm, cancel, or reschedule
- System update: Response writes back to the EHR in real time
Omnichannel Delivery
Patients receive reminders through their preferred channel:
- Voice calls: Natural conversation with the AI agent
- SMS: Text messages for quick confirmations (best practice: avoid detailed PHI in standard SMS; route patients to secure portal for sensitive content)
- Secure messaging: End-to-end encrypted channels for detailed information
Patient preferences vary by demographic. Surveys show 48% prefer text messages for appointment alerts, while 75% of millennials consider text reminders beneficial. Yet 64% still prefer phone calls for cancellations or postponements—which is why omnichannel support isn't optional; it's expected.
These channel preferences also shape how reminder sequences need to be structured across the full patient journey.
Full Reminder Sequence Types
Well-configured systems handle multiple touchpoints:
- Immediate booking confirmations
- Staggered reminders (72 hours and 24 hours prior)
- Same-day directions or telehealth links
- Missed-appointment follow-ups
- Waitlist backfill offers when cancellations occur
The Patient Experience Difference
Conversational AI replaces rigid "press 1 to confirm" IVR menus with natural language interaction. Legacy IVR systems suffer 35-45% call abandonment rates—a friction point that directly affects show rates and patient satisfaction.
Migrating to voice AI cuts average handle times from 6.2 to 2.8 minutes, lifts first-call resolution from 68% to 87%, and pushes satisfaction scores from 3.2/5 to 4.5/5. A patient saying "I need to reschedule for next week" gets an immediate, accurate response—no hold music, no menu loops.
Core Technical Safeguards That Define HIPAA Compliance
Business Associate Agreement (BAA)
Any third-party vendor that creates, receives, maintains, or transmits PHI on behalf of a covered entity is a business associate and must sign a BAA—this is a legal requirement under 45 CFR 164.504(e), not a formality. OCR has fined healthcare organizations specifically for operating without a BAA in place.
Critical BAA provisions include:
- Subcontractor flow-down: Vendor ensures any subcontractors agree to the same restrictions
- Breach notification: Vendor reports unauthorized PHI use or disclosure within required timeframes
- Audit rights: Vendor makes internal practices and records available to HHS for compliance determination
Encryption Requirements
The HIPAA Security Rule (45 CFR 164.312) requires technical measures to guard against unauthorized access to ePHI transmitted over electronic networks. Three distinct data states each carry specific requirements:
- Web/API transit: TLS 1.2 minimum with FIPS-based cipher suites (NIST SP 800-52 Rev. 2); TLS 1.3 was mandated by January 1, 2024
- Data at rest: AES-256 is the FIPS-approved algorithm for securing stored sensitive data
- Voice transit: SRTP (RFC 3711) provides confidentiality, message authentication, and replay protection for voice streams
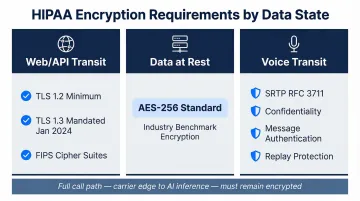
For voice AI, the entire call path—from carrier edge to AI inference layer—must stay encrypted. Vendors routing calls over the public internet rather than private network infrastructure introduce avoidable exposure.
Access Controls and Audit Logs
Controlling who accesses PHI—and proving it—requires two layers of enforcement:
- RBAC (Role-Based Access Control): Limits PHI access by job function, so billing staff can't pull clinical notes and vice versa
- MFA (Multi-factor authentication): Requires a second verification step beyond passwords for all platform access
Immutable audit logs must capture every interaction—caller ID, timestamp, duration, AI decision points—and must be retained for six years under 45 CFR 164.316(b)(2)(i). These logs are your primary evidence during OCR audits and your forensic record after any security incident.
Data Residency and Sovereignty
Several state privacy laws and internal governance policies require patient data to be processed and stored within specific geographic regions. Self-hosting the AI platform—rather than relying on a shared cloud vendor—gives healthcare organizations direct control over where PHI is processed and stored.
Dograh AI supports this through its self-hosting option under an open-source BSD 2-Clause license. Organizations deploy the platform within their own infrastructure or a designated region, keeping PHI within required jurisdictional boundaries and reducing the number of external systems that touch sensitive data—with no vendor lock-in.
TCPA Compliance and Consent Management
HIPAA governs how patient data is handled, but a separate federal law governs how patients are contacted. The Telephone Consumer Protection Act (TCPA), 47 U.S.C. § 227, applies to all automated calls and texts—with individuals able to recover $500 per violation, trebling to $1,500 for willful violations.
A compliant AI system must:
- Record consent status for each patient
- Honor opt-outs instantly
- Observe quiet-hour restrictions
- Maintain an auditable outreach history
How Conversational AI Reduces No-Shows and Administrative Costs
Quantifying the Operational Impact
Automated reminders significantly reduce no-shows. According to MGMA DataDive data, median patient no-show rates in 2021 were 5.1% for primary care, 5.0% for surgical specialties, and 6.0% for nonsurgical specialties. A systematic review demonstrated that patients receiving appointment reminders showed a 34% weighted mean relative reduction in non-attendance from baseline rates.
Adelante Healthcare reduced its no-show rate by 35%, dropping from 18–20% down to 13% for specialist treatment. Patients receive timely outreach, confirm or reschedule in the same interaction, and practices can immediately backfill open slots—without staff involvement.
Staff Cost Savings
Consider a representative cost comparison for 500 reminders per week:
| Manual Calls | Automated AI | |
|---|---|---|
| Cost per contact | ~$0.73 (at $21.91/hr, 2 min/call) | Under $0.10/min (varies by vendor) |
| 500 reminders/week | ~$365/week ($18,980/year) | Significantly lower |
| Operating hours | Business hours only | 24/7, including evenings and weekends |
| Answer rates | Limited by staff availability | Higher during off-hours outreach |
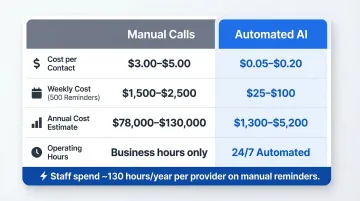
Staff spend approximately 130 hours annually per provider on appointment reminders alone. Eisenhower Imaging Center estimated savings of eight hours per day in staff time after automating this workload—time that flows directly back into patient-facing care.
Multilingual Support and Accessibility
Conversational AI can detect a patient's preferred language and respond accordingly, covering reminders, preparation instructions, and rescheduling without requiring bilingual staff. This improves engagement for diverse patient populations and reduces language-related no-shows—a significant factor in communities with limited English proficiency.
Staff Reallocation
That recovered capacity extends beyond language access. When AI handles high-volume routine outreach, front-desk staff can redirect their time to higher-value work that actually requires human judgment:
- Complex scheduling issues and exception handling
- In-person patient support and check-in coordination
- Care coordination across providers
- Patient advocacy and follow-through on clinical instructions
EHR Integration: Building a Closed-Loop Reminder System
Why EHR Integration Defines True Automation
EHR integration is the difference between genuine automation and a tool that still creates manual work. A properly integrated system reads appointment data directly from the EHR (via FHIR APIs or HL7 v2 standards), triggers outbound reminders based on scheduling rules, and writes the patient's response (confirmed, cancelled, rescheduled) back into the EHR in real time.
This "write-back" capability prevents double-booking and keeps staff working from a single source of truth. Without write-back, someone must manually update appointment statuses after every AI interaction—negating much of the automation benefit.
The Event-Driven Workflow
When a new booking is created or a pre-visit task is triggered in the EHR, the AI automatically initiates the appropriate reminder sequence. For implementation, validate API mappings in a sandbox environment before go-live and monitor integration health with throughput and latency dashboards to catch issues early.
The U.S. EHR Landscape
Which EHR your AI connects to determines which integration path you'll actually use. According to Definitive Healthcare, Epic and Oracle Health (Cerner) dominate both the acute care and ambulatory markets:
| EHR Vendor | Acute Care Market Share | Ambulatory Market Share |
|---|---|---|
| Epic | 37.7% | 43.92% |
| Oracle Health (Cerner) | 21.7% | 25.06% |
| MEDITECH | 13.2% | — |
| athenahealth | — | 2.01% |
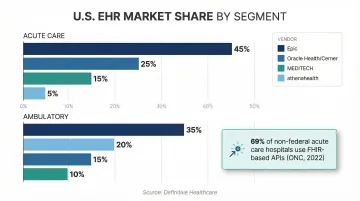
On the standards side, ONC data from 2022 shows that 69% of non-federal acute care hospitals use FHIR-based APIs for patient data access, while 90% of Health Information Exchange organizations routinely receive HL7 v2 ADT messages. In practice, this means most production deployments will rely on one or both standards.
Integration Failures Have Consequences
A 2024 Veterans Administration OIG report illustrates how much is at stake. Investigators found that a scheduling error in a new Oracle EHR system inactivated a high-risk flag — and because the missed appointment was never routed to a rescheduling queue, clinicians failed to evaluate a veteran's mental health, contributing to an overdose.
When evaluating vendors, confirm:
- Coverage of your specific EHR (Epic, Cerner, athenahealth)
- Validation in production healthcare environments — not just sandbox demos
- Native EHR connectivity, since platforms requiring custom development delay deployment and increase your compliance exposure
How to Evaluate and Deploy a HIPAA-Compliant Voice AI Vendor
Non-Negotiable Vendor Criteria
- BAA scope: Must cover all downstream subprocessors, not just the primary vendor
- SOC 2 Type II certification: Third-party validation of security controls (note: SOC 2 aligns closely with HIPAA Privacy Rule requirements but is not equivalent to HIPAA compliance)
- Documented encryption protocols: TLS 1.3 for signaling, SRTP for voice media, AES-256 for data at rest
- Regional data residency options: Ability to control where PHI is processed and stored
- Verifiable audit logging: Immutable logs retained for six years
- Transparent pricing: Per-minute usage rather than flat-rate or bundled pricing models — easier to forecast costs and calculate ROI
Phased Rollout Approach
Start with a single clinic or appointment type to validate technical integration and measure baseline no-show improvement before scaling. Define the KPIs to track from day one:
- Answer rate
- Confirmation rate
- Reschedule rate
- Ultimate show rate
Your platform choice directly affects how quickly you can iterate on these metrics. Dograh AI's open-source architecture lets teams inspect, customize, and extend AI workflows without waiting on vendor release cycles. The self-hosting option eliminates vendor lock-in and provides complete control over data handling, encryption, and security protocols.
Governance and Ongoing Quality Assurance
Designate a project owner responsible for:
- Managing and renewing BAAs as vendor relationships evolve
- Monitoring audit logs for anomalies or access violations
- Reviewing call transcripts and patient feedback to refine reminder scripts
- Keeping AI configurations aligned with current HIPAA policies
Test with frameworks like Dograh's LoopTalk, an AI-driven auto-testing tool that simulates real-world customer scenarios, reducing manual testing effort and improving accuracy before live deployment.
Frequently Asked Questions
Are appointment reminders allowed under HIPAA?
Yes, appointment reminders are permitted under HIPAA. The Privacy Rule's minimum necessary standard allows providers to send reminders using patient contact information. However, the system sending them must handle PHI with all required safeguards (encryption, BAA, access controls, audit logs).
Are voice notes HIPAA compliant?
Voice notes and AI voice calls can be HIPAA compliant when the platform encrypts audio in transit (SRTP) and at rest (AES-256) and restricts access through role-based controls. The platform must also maintain audit logs of every interaction and operate under a signed BAA with the healthcare provider.
Do I need a BAA for an AI appointment reminder service?
Yes, a BAA is legally required under 45 CFR 164.504(e). Any third-party vendor that touches PHI (patient name, appointment details, provider information) is a business associate under HIPAA, and operating without a BAA exposes the covered entity to significant OCR fines — Pagosa Springs Medical Center paid $111,400 for exactly this violation.
What PHI is typically included in appointment reminders?
Standard appointment reminders typically include patient name, appointment date and time, provider or clinic name, and type of service — all identifiers that qualify as PHI under 45 CFR 160.103. Any combination of these triggers HIPAA's full protection requirements.
How much can conversational AI reduce no-show rates?
Well-implemented conversational AI reminders typically reduce no-show rates by 30% or more. Results improve further when the system enables immediate rescheduling and sends staggered multi-touch reminders — Adelante Healthcare cut no-shows from 18-20% down to 13% using this approach.
Can HIPAA-compliant AI appointment reminders integrate with my EHR?
Leading platforms integrate with major EHRs (Epic, Cerner, athenahealth) via FHIR or HL7 APIs, enabling real-time read and write-back of appointment status. However, verify native integration support for your specific EHR before committing to a vendor, as some platforms require custom development.


