
Introduction
Most healthcare front desks operate in controlled chaos. Phones ring nonstop while staff juggle scheduling, insurance verification, prescription refill requests, and in-person patients simultaneously. The numbers tell the story: 23% of inbound calls to medical practices go unanswered, and 41% occur outside standard business hours. For an average multi-physician practice, this translates to approximately $150,000 in lost annual revenue.
Conversational AI can absorb much of that load — but results vary widely depending on how it's deployed. Success hinges on four factors: system configuration, workflow selection, HIPAA compliance, and EHR integration depth.
This guide walks through the exact steps to automate your healthcare front desk with conversational AI, the conditions that must be met first, the parameters that determine success, and the mistakes that cause most deployments to fail.
TL;DR
- Conversational AI automates repetitive tasks like scheduling, FAQs, reminders, and intake, freeing staff for complex patient needs
- HIPAA compliance, EHR integration, and natural conversation handling are non-negotiable for success
- Expect four implementation phases: workflow audit, platform selection, integration, and phased deployment
- Watch three core metrics: response latency, context retention, and escalation logic quality
- High call volumes, after-hours gaps, and understaffed front desks signal the strongest ROI potential
How to Automate Your Healthcare Front Desk with Conversational AI
Step 1: Audit Your Front Desk Workflows Before Touching Any Technology
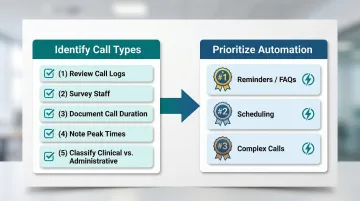
Map every inbound and outbound call type your front desk handles—scheduling, prescription refills, insurance questions, appointment reminders, after-hours triage. Identify the top 3–5 by volume. These are your highest-priority automation targets.
Why this matters: 76% of front-desk phone tasks fall into just two categories—eligibility/prior authorization (45%) and scheduling (31%). Automating these two workflows alone addresses over 75% of call volume.
Start your audit by:
- Reviewing call logs for the past 30 days to identify volume patterns
- Surveying front desk staff about which calls consume the most time
- Documenting average call duration by type
- Noting peak call times and after-hours demand
- Identifying which calls require clinical judgment versus administrative processing
The highest-volume, most structured workflows—reminders and FAQ handling—should be automated first. Complex or emotionally sensitive calls like urgent triage or billing disputes should be tackled only after the AI is calibrated and proven.
Step 2: Select a HIPAA-Compliant Conversational AI Platform
HIPAA compliance is non-negotiable. Your platform must provide a signed Business Associate Agreement (BAA), data encryption in transit and at rest, audit logging, and SOC 2 certification.
Critical compliance requirements:
- Cloud Service Providers storing encrypted ePHI are Business Associates, even if they lack the decryption key. Execute a BAA before deployment — Oregon Health & Science University paid $2.7 million for skipping this step.
- Encrypt all data at rest and in transit using NIST-compliant methods
- Require full audit logging — every interaction involving ePHI must be recorded and reviewable
- For practices with strict data sovereignty requirements, on-premise deployment eliminates third-party data handling entirely — Dograh AI offers full on-premise control under a BSD 2-Clause open-source license
Functional criteria to evaluate:
- EHR/practice management integration capability
- Natural language understanding quality
- Multi-call handling capacity
- Escalation workflow design
- Transparent pricing without hidden per-minute STT/TTS/LLM charges
Platforms using a bring-your-own-keys model eliminate platform markup and provide complete cost transparency—you see exactly what you pay to each vendor without hidden intermediary charges.
Step 3: Configure Your AI Agent and Integrate It with Your EHR
Configuration involves loading practice-specific FAQs, hours, provider schedules, accepted insurance, and escalation rules. What you feed the AI determines response accuracy.
EHR integration determines whether your AI agent completes transactions or just logs them. The AI must read real-time schedule availability, confirm patient identity, and write back booking confirmations or refill requests. Without bidirectional integration, staff still manually process every AI-captured request — adding a queue instead of eliminating one.
Integration depth matters:
| Integration Type | Capabilities | Operational Impact |
|---|---|---|
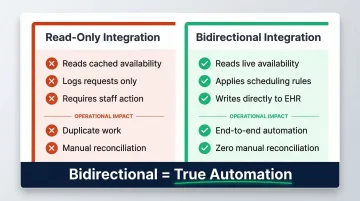
| Read-Only | Reads cached availability; logs requests; requires staff action to create appointments | Creates duplicate work; forces manual reconciliation |
| Bidirectional | Reads live availability; applies scheduling rules; writes confirmed appointments directly into EHR in real time | Completes transactions end-to-end without staff involvement |
Bidirectional integration is the threshold for true automation. Read-only setups require a staff member to act on every AI interaction — the call volume drops, but the appointment-entry workload doesn't.
Step 4: Test with Real Scenarios, Train Staff, and Deploy in Phases
Start with one high-volume, low-risk workflow: appointment reminders or FAQ answering. Monitor accuracy and escalation rates for 2–4 weeks before expanding to scheduling and intake.
Skipping phased testing is one of the most common failure points. Patients encounter untested AI behavior, and staff receive escalated calls without the context or process to handle them cleanly.
What "ready to expand" looks like:
Gartner predicts that by 2029, agentic AI will autonomously resolve 80% of common customer service issues. Currently, the average first call resolution rate in healthcare call centers sits at 52%. Target at least 70% AI resolution without human escalation before scaling automation to additional workflows.
Phased deployment steps:
- Weeks 1-2: Deploy for appointment reminders only; measure completion rate and patient feedback
- Weeks 3-4: Add FAQ handling for hours, directions, insurance accepted; track escalation frequency
- Weeks 5-8: Expand to appointment scheduling; monitor booking accuracy and no-show rates
- Weeks 9+: Add intake forms and prescription refill routing based on performance data
Train staff on how to receive escalations with full call context. When the AI hands off a call, the receiving staff member should see the complete transcript and patient information—no repetition required.
When Should You Automate Your Healthcare Front Desk with Conversational AI?
Conversational AI front desk automation is not equally valuable for every practice. ROI is highest when specific operational signals are present. Deploying too early — or for the wrong reasons — leads to underuse and wasted spend.
Conditions indicating readiness and strong ROI:
- Fielding 50+ calls per day — volume is the clearest predictor of strong automation ROI
- Missing 15%+ of inbound calls — each missed call is potential revenue walking out the door
- 41% of patient calls come in after hours (outside 8 AM–5 PM weekdays) — automation captures demand your staff can't cover
- Front desk staff burning time on the same repetitive questions, flagging burnout
- High front-office turnover — 71% of physicians cite clerical burdens as a top driver of burnout, and the front desk bears most of that load

Scenarios where conversational AI is a poor immediate fit:
- Fewer than 20 daily calls — the investment won't pencil out at low volume
- Workflows dominated by emotionally sensitive or urgent clinical calls — start with reminders and FAQs, not full automation
- No viable EHR integration — without bidirectional connection to your practice management system, the AI can't complete transactions autonomously, and staff end up processing everything manually anyway
If your practice hits two or more of the readiness signals above, full front desk automation is worth evaluating. If not, a scoped deployment — reminders and routine FAQs — is a lower-risk starting point.
Key Parameters That Affect Results When Using Conversational AI at the Healthcare Front Desk
Two practices can deploy the "same" conversational AI and see drastically different outcomes. The difference lies in how these specific parameters are configured.
Response Latency
In voice conversations, delays exceeding 500ms cause patients to think the call dropped or speak over the AI, breaking conversation flow. Human conversational turn-taking gaps average around 200 milliseconds, and delayed responses are often interpreted as less cooperative or hesitant.
That gap matters in practice. High-latency AI produces higher call abandonment rates and more manual escalations — both outcomes that defeat the purpose of automation. ITU-T standards suggest highly interactive tasks benefit from delays below 150ms, with a hard ceiling of 400ms one-way delay. Systems operating at sub-500ms response times produce measurably more natural patient interactions.
EHR Integration Depth
Not all EHR integrations are equal. Superficial integration — where the AI reads schedule data but cannot write back — forces staff to manually reconcile every AI-booked appointment.
The contrast between integration depths is significant:
- Shallow integration: AI reads schedules only; staff must manually enter bookings, creating a dual-entry workflow that increases admin burden
- Deep bidirectional integration: AI books, reschedules, logs call notes, and updates patient records in real time — no manual reconciliation required
Deep integration is the threshold at which scheduling automation actually reduces staff workload.
Conversation Context Retention
Patients rarely communicate in neat, linear sequences. They interrupt, change topics, and circle back to earlier parts of the call. An AI that loses context after a few exchanges forces patients to repeat themselves — consistently one of the top drivers of caller frustration and early hang-ups.
Context retention window varies significantly across platforms, measured in conversation turns or total call minutes. Longer retention allows the AI to handle complex multi-part requests without breaking down. Dograh AI's multi-agent architecture supports 45+ minute context retention, which covers even extended scheduling discussions and multi-question calls without losing thread.
Escalation Logic Design
Escalation rules — which call types trigger a human handoff and how that handoff executes — determine patient safety and satisfaction more than any other parameter. Poor escalation design is the most common source of serious outcomes in healthcare AI deployments.
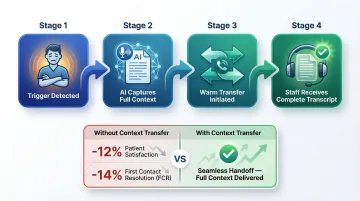
Well-designed escalation passes the full call transcript and patient context to the receiving staff member so the patient never has to repeat themselves. When a customer is transferred without context, satisfaction drops 12% and first call resolution drops 14%.
Call types that should always escalate:
- Distressed or upset patients
- Urgent clinical concerns
- Complex billing disputes
- Requests requiring clinical judgment
- Patients explicitly requesting a human
Configure these triggers before deployment. Test them during phased rollout. Adjust based on escalation rate monitoring.
Common Mistakes When Deploying Conversational AI at the Healthcare Front Desk
Most deployment failures follow a predictable pattern: shortcuts taken at the start create compounding problems later. Here are the five mistakes that derail healthcare AI rollouts most often.
Skipping or rushing the compliance review:
Deploying a conversational AI platform without a signed BAA, confirming HIPAA-compliant data storage, or verifying audit trail capabilities exposes the practice to significant regulatory risk. Compliance verification must be complete before any PHI enters the system.
Enforcement actions prove this: North Memorial Health Care paid $1.55 million for failing to obtain a signed BAA before granting database access to 289,904 patient records. Raleigh Orthopaedic Clinic paid $750,000 for handing over PHI of 17,300 patients to a vendor without executing a BAA first.
Treating AI deployment as a set-and-forget installation:
AI agents require ongoing monitoring: tracking escalation rates, reviewing transcripts for errors, updating FAQs as policies change, and retraining on edge cases. Practices that skip this maintenance phase see accuracy drop within weeks of launch.
Choosing the wrong workflows to automate first:
Starting with high-complexity or emotionally sensitive call types before the AI is calibrated is a common failure. Begin with the highest-volume, most structured workflows like reminders and FAQ handling. Expand to scheduling and intake only after proving accuracy and escalation logic in lower-risk scenarios.
Ignoring patient communication about the AI transition:
Patients who are surprised to reach an AI—without being told upfront they are speaking with an AI assistant—report lower satisfaction and trust. Best practice is to disclose AI identity at the start of every call and give patients an easy path to a human if preferred.
Research shows 55% of patients are comfortable with AI for routine tasks, and over 75% remain satisfied when AI authorship is disclosed upfront.
A brief disclosure like "You're speaking with an AI assistant designed to help schedule appointments" upholds patient autonomy without meaningfully impacting satisfaction scores.
Conclusion
Automating the healthcare front desk with conversational AI works best when the foundation is solid before go-live. Three conditions consistently separate successful deployments from abandoned ones:
- Workflow audit first — map current front desk processes before selecting any tool
- True HIPAA compliance — self-hosted or BAA-backed deployment with bidirectional EHR integration
- Phased rollout with monitoring — treat it as an ongoing program, not a one-time installation
Most failures trace back to skipped compliance steps, shallow EHR integration, or poorly configured escalation logic — not the technology itself. Getting these right is what separates practices that achieve measurable ROI from those that abandon the tool within months.
Platforms with self-hosted deployment options, transparent pricing, and bidirectional EHR integration — such as Dograh AI's open-source platform, licensed under BSD 2-Clause — give practices the data sovereignty and cost control required for long-term automation success.
Frequently Asked Questions
What is conversational AI in healthcare?
Conversational AI in healthcare refers to AI systems that conduct natural, two-way spoken or text-based conversations with patients to handle tasks like scheduling, answering questions, and collecting intake information — unlike older IVR systems that required button-press navigation through rigid menus.
Are there HIPAA-compliant conversational AI solutions for healthcare front desks?
Yes — HIPAA-compliant conversational AI solutions are widely available. Compliance requires a signed Business Associate Agreement, encrypted data handling, and audit logging. Self-hosted platforms like Dograh AI provide the highest level of data control, keeping PHI entirely within the practice's own infrastructure.
Which conversational AI tools are best for healthcare front desks?
The best tools combine HIPAA compliance, bidirectional EHR integration, natural conversation quality, and transparent pricing. Open-source and self-hostable platforms like Dograh AI offer an alternative to proprietary SaaS vendors for practices that need full data sovereignty without recurring platform fees or vendor lock-in.
How long does it take to implement conversational AI for a medical front desk?
Implementation timelines typically range from a few days to several weeks depending on the platform, EHR integration complexity, and how many workflows are being automated. Phased deployments that start with one workflow can go live much faster than full front desk automation from day one.
Can conversational AI integrate with my existing EHR system?
Most healthcare-focused conversational AI platforms integrate with major EHR and practice management systems, but depth varies. Practices should confirm whether the integration is read-only or bidirectional — only bidirectional integration eliminates manual reconciliation work.
What happens when conversational AI cannot handle a patient's request?
Well-configured AI agents recognize their limitations and escalate to a human staff member, passing the full call transcript and patient context so the patient does not need to repeat themselves. Look for platforms that preserve conversation context and route clearly — these details directly affect patient satisfaction.


