
Introduction
Property and casualty carriers hold decades of policyholder data locked inside legacy systems — on-premise Guidewire, Duck Creek, Majesco, and batch-era mainframes — while demand for AI voice agents handling FNOL, claims status, and renewals has moved from pilot project to board-level priority.
The pressure is real: 74% of insurance companies still rely on outdated legacy technology for core processes, while policyholders increasingly expect the instant, conversational service they get from tech companies.
The core problem is that integrating a real-time AI voice layer with systems designed for overnight batch processing isn't a software swap. These platforms were built before APIs existed, when sub-second response times were never a requirement.
Voice AI needs to query and update records within 200–500ms to maintain natural conversation flow. Legacy architectures can take several seconds just to authenticate a session.
This guide walks through integration patterns that work inside real P&C environments: how to bridge the latency gap, manage regulatory constraints, and sequence a rollout that doesn't require ripping out core systems.
TLDR
- Legacy P&C systems lack real-time APIs and were built for batch processing — integration requires architectural workarounds, not system replacement
- Middleware, API wrappers, and event-driven pipelines close the gap in 4–8 weeks — versus 12–24 months for full platform migrations
- NAIC guidelines (24 states), PCI DSS v4.0.1, and state-level AI regulations must be built into integration architecture from day one
- Start with read-only, low-risk workflows (claims status) before expanding to write-back operations (FNOL intake, policy endorsements)
- Self-hosted voice AI keeps legacy systems off external cloud endpoints, reducing both security exposure and compliance risk
Why Legacy P&C Systems Block Voice AI Integration
The Batch Processing Architecture Problem
Most mid-to-large carriers run on-premise Guidewire, Duck Creek, Majesco, or fully custom policy administration systems built before the API era. These platforms handle billions in premiums but were designed for batch throughput — not sub-second real-time queries. Policy updates process overnight. Billing cycles run once daily.
Voice AI requires end-to-end response latency under 500ms to feel natural. That budget disappears fast:
- Speech recognition: 40–300ms
- LLM processing: 100–400ms
- Text-to-speech generation: 50–250ms
When a legacy system takes 2–3 seconds just to authenticate a session and return policyholder data, callers notice the lag immediately — and trust in the agent drops.
The Missing API Layer
Legacy P&C systems typically expose SOAP-based web services, CSV exports, or proprietary interfaces — not REST APIs. Many require terminal emulation or screen scraping for any external access at all. Voice AI needs to query and update records within 200–500ms windows, which batch architectures simply cannot support natively.
The integration timelines reflect this gap. Direct platform deployments for Guidewire typically run 12–24 months; Duck Creek implementations range from 9–18 months. Neither timeline is compatible with a voice AI rollout moving at product speed.
Data Silos Across the P&C Stack
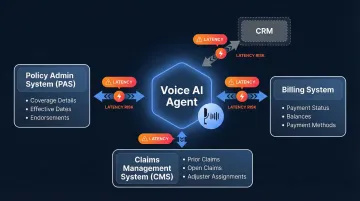
Policyholder data is fragmented across policy admin (PAS), claims management (CMS), billing, and separate CRM systems. A voice agent handling FNOL needs to pull and correlate data from at least three systems simultaneously:
- Policy Admin System: Coverage details, effective dates, endorsements
- Claims Management: Prior claims history, open claims, adjuster assignments
- Billing System: Payment status, outstanding balances, payment methods
Each system has its own data schema, authentication method, and performance characteristics. Coordinating real-time queries across this fragmented landscape without introducing latency or data consistency issues is a core integration challenge.
The Security Perimeter Challenge
Many legacy P&C systems run on isolated internal networks specifically to meet compliance and security requirements. Opening these systems to cloud-hosted AI introduces attack surface that security and compliance teams will immediately flag. Traditional integration approaches require exposing internal databases to external endpoints, creating audit exceptions and expanding PCI DSS scope.
The Human Dimension
Legacy system administrators who have maintained these platforms for years often resist integration projects. They know where the landmines are: the undocumented API behaviors, the tables that lock under concurrent access, the batch jobs that fail if queries run during processing windows. Getting their input early — not after architecture decisions are made — is what separates integrations that ship from ones that stall in change management for quarters.
Integration Patterns That Work for P&C Environments
API Wrapper Layer for Read-Only Access
For P&C systems with some modern interfaces, a thin API wrapper translates legacy SOAP or proprietary calls into REST endpoints. This is the fastest pattern — typically 4–8 weeks — and lowest risk.
Best for:
- Claims status inquiries
- Policy coverage lookups
- Premium balance checks
How it works: The wrapper sits between the voice AI and legacy system, caching frequently accessed data and translating modern REST calls into whatever protocol the legacy system speaks. The voice agent never touches the core system directly.
Middleware and Event-Driven Architecture
For carriers with multi-system environments (PAS + CMS + billing all in play), a middleware layer using a message bus like Kafka or RabbitMQ decouples the voice AI from backend systems.
Key advantages:
- The agent reads from a normalized data layer
- Writes queue asynchronously, so slow legacy systems don't stall live calls
- Middleware handles data correlation across systems
Change Data Capture (CDC) tools like Debezium track database changes in real-time, streaming updates into Kafka. Guidewire's Data Platform uses this exact pattern, streaming CDC data from ClaimCenter and PolicyCenter with near-zero latency. This approach reduces integration timelines from 12–24 months to 8–12 weeks.
Database Replication for Read-Heavy Workflows
For use cases where the voice agent primarily retrieves data — claims status, policy details, coverage explanations — creating a near-real-time read replica of critical tables gives the AI fast, reliable data access without touching live production systems.
Implementation approach:
- Oracle GoldenGate, AWS DMS, or similar CDC tools keep replicas current
- Voice AI queries the replica, not production
- Writes still route through legacy system APIs
This pattern works well for Phase 1 deployments where you need fast query response but can't risk impacting production operations. For carriers with strict data residency requirements, self-hosted deployment adds another layer of control.
Self-Hosted Deployment for Network Security
Voice AI platforms that deploy on-premise or in a private cloud environment remove the need to route policyholder voice data through external cloud endpoints. The AI lives inside the same network perimeter as the legacy systems it queries.
Dograh AI's open-source architecture supports both cloud and on-premise deployment, keeping voice data and transcripts within the carrier's existing security perimeter. Because it's self-hostable, carriers retain full control over data sovereignty without routing sensitive policyholder information through third-party infrastructure. This simplifies HIPAA and state data residency compliance considerably.
Integration Pattern Comparison
| Pattern | Implementation Time | Integration Risk | Best Use Case |
|---|---|---|---|
| API Wrapper | 4–8 weeks | Low | Claims status, policy lookup |
| Middleware / Event-Driven | 8–12 weeks | Medium | Multi-system FNOL intake |
| Database Replication | 6–10 weeks | Low | High-volume read queries |
| Self-Hosted Deployment | 4–8 weeks | Low | Regulated environments, data residency requirements |

Compliance, Security, and Data Sovereignty in P&C Voice AI
The NAIC 2023 AI Model Bulletin
Adopted on December 4, 2023, the NAIC Model Bulletin on the Use of Artificial Intelligence Systems requires insurers to demonstrate that AI systems operating in claims and customer service workflows are auditable, explainable, and governed. Voice AI integrations must produce full call transcripts, interaction logs, and audit trails that satisfy both internal QA and regulatory examination.
As of early 2025, 24 states have adopted the NAIC Model Bulletin or issued analogous guidance, including Alaska, Connecticut, Illinois, Pennsylvania, and Wisconsin. Key requirements include maintaining inventories of AI models, ensuring auditability of AI decisions, and conducting rigorous due diligence on third-party AI vendors.
Practical implications:
- Every voice interaction that informs a claims decision must be logged
- Integration design should include structured logging at the middleware layer, not just call recordings
- Audit logs must link to the carrier's existing compliance infrastructure
Dograh AI's SOC 2, HIPAA, GDPR, and PCI DSS certifications, combined with self-hosting options, give carriers a complete audit trail and direct control over where sensitive voice data is processed and stored.
PCI DSS v4.0.1 and Voice-Captured Payment Data
Policyholders often make premium payments over the phone. Voice AI that captures card data during calls must meet PCI DSS scope. Under PCI DSS v4.0.1, traditional "pause-and-resume" call recording is effectively obsolete — it's prone to human error and leaves the agent environment in scope.
Recommended approach: Dual-Tone Multi-Frequency (DTMF) masking or suppression intercepts keypad tones, replacing them with flat sounds before they reach the agent or recording system. This removes the telephony environment and agent desktop from PCI DSS scope.
Carriers must verify their voice AI platform carries PCI DSS certification before going live on billing workflows.
Data Residency Requirements
Some P&C carriers, particularly those serving regulated lines or government contracts, must keep policyholder data within specific geographic boundaries. Integration architecture must account for where voice data is processed and stored, not just where core systems sit.
Self-hostable platforms give carriers direct control over data residency. Rather than routing voice traffic through external cloud providers' infrastructure, carriers can deploy the entire voice AI stack within their own data centers or cloud regions, ensuring compliance with state insurance department requirements and NYDFS 23 NYCRR 500.
Mapping P&C Voice Workflows to Integration Depth
Low Complexity: Read-Only Workflows
Claims status inquiries and policy coverage lookups require only read access to CMS and PAS. These are the right starting point because they generate immediate policyholder value — eliminating hold times — while posing minimal risk to legacy data integrity.
What makes them ideal:
- 58% of inbound calls at a regional P&C insurer were simple claims status checks
- Average handle time drops from 6.5 minutes (human) to under 3 minutes (AI)
- API wrapper or read replica is sufficient
- No regulatory approval needed for read-only access
One regional carrier reduced claims inquiry call volume by 68% and saved $612,000 annually by deploying a voice agent integrated with Guidewire ClaimCenter for read-only status checks.

Once read-only workflows are stable and validated, the next tier introduces write operations — and with them, authentication requirements and data schema discipline.
Medium Complexity: Authenticated Read-Write
FNOL intake requires the voice agent to capture structured incident data, verify policy coverage, and write a new claim record to the CMS. This demands authenticated write-back integration and structured data mapping between conversation output and the legacy system's data schema.
Key requirements:
- Identity verification before write operations
- Structured data capture (incident date, location, vehicle details, injury description)
- Schema mapping from conversation to legacy system fields
- Middleware patterns for asynchronous queuing
Human-handled FNOL calls run 15–18 minutes and cost approximately $25 in labor. Voice AI can handle the same intake in 5–6 minutes at roughly $2 per call, an 87% reduction in handle time and a 92% drop in cost-per-call.
With FNOL patterns established, teams are ready to take on workflows that span multiple systems in a single transaction.
High Complexity: Multi-System Write Workflows
Policy endorsements and payment processing require identity verification, eligibility checks across PAS and billing, and transactional writes across multiple systems. These should only be tackled after simpler workflows are stable.
Data flow example:
- Voice agent captures endorsement request
- Queries PAS for current policy status and coverage
- Checks billing system for payment status
- Validates endorsement rules in policy engine
- Writes endorsement request to PAS
- Updates billing for premium adjustment
- Triggers confirmation email/SMS

Each system call is a potential failure point — design compensating transactions at steps 5 and 6 so a billing rejection automatically voids the PAS write and returns the agent to a clean state.
A Phased Rollout Roadmap for P&C Voice AI Integration
Rushing a voice AI deployment into production rarely ends well — especially against legacy P&C systems with limited APIs and brittle data models. A phased rollout lets you validate architecture, build stakeholder confidence, and expand only when each stage proves stable.
Phase 1: Pilot (Weeks 1–6)
Objective: Validate integration architecture and data accuracy in a controlled environment.
Key activities:
- Select one read-only use case (claims status is ideal)
- Connect voice AI to a read replica or API wrapper of the CMS
- Test internally with real data in staging environment
- Validate data accuracy against known outputs before routing any live calls
- Establish baseline metrics: query latency, data retrieval accuracy, edge case identification
Success criteria: Sub-500ms query response time, 95%+ data accuracy, documented edge cases.
Phase 2: Limited Production (Weeks 7–12)
Objective: Prove value with real policyholders while maintaining human oversight.
Key activities:
- Route 10–20% of real inbound calls to the voice AI agent
- Monitor containment rate, data retrieval accuracy, and escalation triggers
- Collect call transcripts to identify edge cases and legacy system response time issues
- Establish human-in-the-loop fallbacks for complex scenarios
- Track AHT, CSAT, and cost per interaction
Success criteria: 40%+ containment rate, CSAT scores within 5% of human baseline, no production system impact.
These targets are achievable: mature deployments have reached a 53% automation rate (Aspire General Insurance), with 60–80% claims intake automation within six months. Hitting Phase 2 benchmarks signals you're ready to expand.
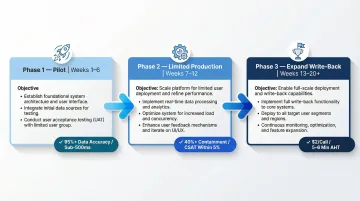
Phase 3: Expand to Write-Back Workflows (Weeks 13–20+)
Objective: Scale to high-value workflows that require authenticated write operations.
Write-back workflows carry more risk than read-only ones — a failed write to a legacy CMS can corrupt a claim record or drop a FNOL entirely. Plan for failure before it happens.
Key activities:
- Add FNOL intake or policy inquiry workflows that require authenticated write-back
- Introduce middleware for asynchronous queuing so legacy system latency doesn't affect call quality
- Implement and test rollback procedures — reviewed and approved by legacy system administrators — before go-live
- Scale gradually to 50%+ of traffic
Success criteria: AHT reduction to 5–6 minutes for FNOL, cost per call reduced to $2, zero production incidents caused by voice AI writes.
Frequently Asked Questions
Can AI voice agents integrate with Guidewire, Duck Creek, or Majesco without a full system rebuild?
Yes. Pre-built API connectors or wrapper layers can connect modern voice AI to these platforms without replacing them. The key is matching the integration pattern to the system's available interfaces — REST, SOAP, or direct DB access via CDC streaming — to achieve 4–8 week deployment timelines instead of 12–24 month migrations.
How long does it typically take to integrate AI voice agents with legacy P&C systems?
Timeline depends on the integration pattern and use case scope. Read-only workflows via API wrappers can go live in 4–8 weeks, while full write-back FNOL workflows through middleware typically take 8–12 weeks. Direct core system replacements take 12–24 months but aren't necessary for voice AI integration.
How do you maintain regulatory compliance when AI voice agents access sensitive policyholder data?
Compliance requires full audit logs, PCI DSS certification for payment-capturing workflows, and alignment with the NAIC 2023 AI Model Bulletin (now adopted by 24 states). Data residency is managed through deployment architecture — self-hosted or on-premise setups keep voice data within the carrier's own security perimeter.
What P&C voice AI workflows should insurers automate first?
Claims status and policy coverage lookups are ideal starting points. They represent high call volume (58% of inbound calls at some carriers), low integration risk (read-only access), and immediate ROI through reduced hold times and adjuster interruptions. AHT drops from 6.5 minutes to under 3 minutes.
Does self-hosting a voice AI platform reduce the compliance burden for P&C carriers?
Yes. Self-hosting eliminates third-party data handling exposure and gives compliance teams direct auditability over every policyholder interaction — a practical requirement under NAIC and state insurance department oversight. It also removes vendor dependency from your regulatory audit trail.
How should carriers handle real-time data needs when legacy P&C systems are batch-oriented?
Use database replication with CDC sync to create a near-real-time read layer that voice agents can query without touching production systems. For writes, implement asynchronous queuing through middleware so legacy latency doesn't affect live conversations — write-back operations can execute off-peak when needed.


